The coccygeus muscle or ischiococcygeus is a muscle of the pelvic floor located posterior to levator ani and anterior to the sacrospinous ligament.
| Coccygeus muscle | |
|---|---|
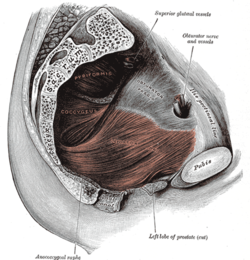 Left levator ani from within. | |
| Details | |
| Origin | Sacrospinous ligament and ischial spine |
| Insertion | Lateral margin of coccyx and related border of sacrum |
| Nerve | Pudendal nerve; sacral nerves: S4, S5[1] or S3-S4[2] |
| Actions | Pulls coccyx forward after defecation, closing in the back part of the outlet of the pelvis |
| Identifiers | |
| Latin | musculus coccygeus |
| TA98 | A04.5.04.011 |
| TA2 | 2412 |
| FMA | 19088 |
| Anatomical terms of muscle | |
Structure
editThe coccygeus muscle is posterior to levator ani and anterior to the sacrospinous ligament in the pelvic floor. It is a triangular plane of muscular and tendinous fibers. It arises by its apex from the spine of the ischium and sacrospinous ligament.[3][4] It is inserted by its base into the margin of the coccyx and into the side of the lowest piece of the sacrum.[3][4]
In combination with the levator ani, it forms the pelvic diaphragm.[5]
The pudendal nerve runs between the coccygeus muscle and the piriformis muscle, superficial to the coccygeus muscle.[6]
Nerve supply
editThe coccygeus muscle is innervated by the pudendal nerve, which runs between it and the piriformis muscle.[7]
Function
editThe coccygeus muscle assists the levator ani and piriformis muscle in closing in the back part of the outlet of the pelvis.[8] This helps to support the vagina in women, and the other pelvic organs.[8]
See also
editReferences
editThis article incorporates text in the public domain from page 424 of the 20th edition of Gray's Anatomy (1918)
- ^ Essential Clinical Anatomy. K.L. Moore & A.M. Agur. Lippincott, 2 ed. 2002. Page 217
- ^ "uams.edu". Archived from the original on 2007-12-16. Retrieved 2007-12-09.
- ^ a b Ho, MAT H.; Bhatia, NARENDER N. (2007-01-01), Lobo, Rogerio A. (ed.), "CHAPTER 51 - Lower Urinary Tract Disorders in Postmenopausal Women", Treatment of the Postmenopausal Woman (Third Edition), St. Louis: Academic Press, pp. 693–737, doi:10.1016/b978-012369443-0/50063-6, ISBN 978-0-12-369443-0, retrieved 2021-02-07
- ^ a b Sokol, Andrew I.; Walters, Mark D. (2007-01-01), Sokol, Andrew I.; Sokol, Eric R. (eds.), "Chapter 23 - Pelvic Organ Prolapse and Pelvic Floor Dysfunction", General Gynecology, Philadelphia: Mosby, pp. 543–581, doi:10.1016/b978-032303247-6.10023-1, ISBN 978-0-323-03247-6, retrieved 2021-02-07
- ^ Barone, William R.; Abramowitch, Steven D.; Moalli, Pamela A. (2015-01-01), Badylak, Stephen F. (ed.), "Chapter 13 - Host Response to Biomaterials for Pelvic Floor Reconstruction", Host Response to Biomaterials, Oxford: Academic Press, pp. 375–423, doi:10.1016/b978-0-12-800196-7.00013-x, ISBN 978-0-12-800196-7, retrieved 2021-02-07
- ^ Bennett, Richard C.; Peters, Kenneth M. (2008-01-01), Raz, Shlomo; Rodríguez, Larissa V. (eds.), "Chapter 24 - PUDENDAL NERVE STIMULATION", Female Urology (Third Edition), Philadelphia: W.B. Saunders, pp. 284–289, doi:10.1016/b978-1-4160-2339-5.50073-2, ISBN 978-1-4160-2339-5
- ^ H. Kim, Daniel; A. Murovic, Judith (2008-01-01), Kim, Daniel H.; Midha, Rajiv; Murovic, Judith A.; Spinner, Robert J. (eds.), "11 - Lower extremity nerve injuries", Kline and Hudson's Nerve Injuries (Second Edition), Edinburgh: W.B. Saunders, pp. 209–278, doi:10.1016/b978-0-7216-9537-2.50019-0, ISBN 978-0-7216-9537-2, retrieved 2021-02-07
- ^ a b Muir, Tristi W. (2008-01-01), Raz, Shlomo; Rodríguez, Larissa V. (eds.), "Chapter 74 - POSTERIOR WALL PROLAPSE: SEGMENTAL DEFECT REPAIR", Female Urology (Third Edition), Philadelphia: W.B. Saunders, pp. 729–736, doi:10.1016/b978-1-4160-2339-5.50123-3, ISBN 978-1-4160-2339-5, retrieved 2021-02-07
External links
edit- Anatomy photo:43:16-0103 at the SUNY Downstate Medical Center - "The Female Pelvis: Muscles of the Pelvic Diaphragm"
- Cross section image: pelvis/pelvis-e12-15—Plastination Laboratory at the Medical University of Vienna
- pelvis at The Anatomy Lesson by Wesley Norman (Georgetown University) (femalepelvicdiaphragm, malepelvicdiaphragm)
- Coccyx pain, tailbone pain, coccydynia (Peer-reviewed medical chapter, available free online at eMedicine)