This article includes a list of general references, but it lacks sufficient corresponding inline citations. (August 2020) |
Pott's disease, or Pott disease, named for British surgeon Percivall Pott who first described the symptoms in 1799,[1] is tuberculosis of the spine,[2][3] usually due to haematogenous spread from other sites, often the lungs. The lower thoracic and upper lumbar vertebrae areas of the spine are most often affected.
| Pott's disease | |
|---|---|
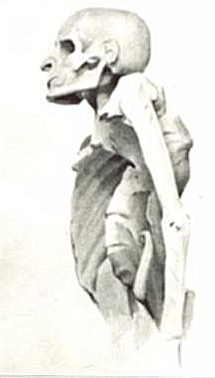 | |
| Tuberculosis of the spine in an Egyptian mummy | |
| Specialty | Rheumatology |
| Symptoms | Pott's spine, tuberculous spondylitis, spinal tuberculosis |
| Diagnostic method | Radiograph, Bone scan, MRI |
| Named after | Percivall Pott |
It causes a kind of tuberculous arthritis of the intervertebral joints. The infection can spread from two adjacent vertebrae into the adjoining intervertebral disc space. If only one vertebra is affected, the disc is normal, but if two are involved, the disc, which is avascular, cannot receive nutrients, and collapses. In a process called caseous necrosis, the disc tissue dies, leading to vertebral narrowing and eventually to vertebral collapse and spinal damage. A dry soft-tissue mass often forms and superinfection is rare.
Spread of infection from the lumbar vertebrae to the psoas muscle, causing abscesses, is not uncommon.[4]
Diagnosis
editThe most common and earliest clinical symptom of Pott's Disease is back pain, often associated with local tenderness, worsening muscle spasms along the spine, and focal edema. These symptoms can lead to limited and painful movement in all directions of the spine.
The second most common clinical symptom is neurological deficits, which can vary depending on the level of the spine affected. An infection in the neck area can cause nerve problems affecting both the arms and legs, while an infection in the lower back typically affects only the legs and the area around the tailbone.
In the early stages of Pott’s Disease, imaging techniques such as CT scans, MRIs, or plain radiographs are ordered. For a radiolucent lesion to appear on a plain X-ray, there must be a 30% loss of bone mineral, making it difficult to diagnose the early stages of Pott's Disease with a plain radiograph. CT (computed tomography) is often used as a guide for biopsy. Overall, it is widely documented that MRI is superior to plain radiographs in diagnosing Pott’s Disease.
Initial suspicion of Pott’s Disease is usually based on clinical symptoms and imaging findings, but a definitive diagnosis requires isolating the organism by culture, identifying it, and determining its drug susceptibility. The typical lab procedure for clinical specimens involves an AFB (acid-fast bacilli) stain.
The ESR (erythrocyte sedimentation rate) and CRP (C-reactive protein) are also used as biomarkers for spinal tuberculosis.
Other labs include:
- Blood tests
- Complete blood count: leukocytosis
- Elevated erythrocyte sedimentation rate: >100 mm/h
- Tuberculin skin test
- Tuberculin skin test (purified protein derivative [PPD]) results are positive in 84–95% of patients with Pott disease who are not infected with HIV.
- Radiographs of the spine
- Radiographic changes associated with Pott disease present relatively late. These radiographic changes are characteristic of spinal tuberculosis on plain radiography:
- Lytic destruction of anterior portion of vertebral body
- Increased anterior wedging
- Collapse of vertebral body
- Reactive sclerosis on a progressive lytic process
- Enlarged psoas shadow with or without calcification
- Additional radiographic findings may include:
- Vertebral end plates are osteoporotic
- Intervertebral disks may be shrunken or destroyed
- Vertebral bodies show variable degrees of destruction
- Fusiform paravertebral shadows suggest abscess formation
- Bone lesions may occur at more than one level
- Bone scan
- Computed tomography of the spine
- Bone biopsy
- MRI
Clinical presentation
editThe onset of symptoms is gradual and disease progresses slowly.[5] The duration of symptoms before diagnosis ranges from 2 weeks to several years, The average period was at least 12 months, but it has recently decreased to 3 and 6 months.[5] Presentation depends on disease stage, location, and complications such as neurological deficits and abscesses.[5]
Non-spinal symptoms include weakness, loss of appetite, weight loss, evening fever, and night sweats.[5] Clinical findings include back pain, paraparesis, kyphosis, sensory disturbances, and bowel and bladder dysfunction.[5] Signs of associated extraskeletal tuberculosis include cough, expectoration, swollen lymp nodes, diarrhea, and abdominal swelling.[5]
The earliest and most common symptom is back pain, which worsens with activity.[5][6] Muscles relax when asleep which causes pain. As the infection progresses, the pain becomes more severe leading to para-spinal muscle spasms.[5] The spasms cause all spinal movements to be restricted and painful.[5]
The second most common symptom is neurological deficits which depends on the location of the infection.[6] If the cervical spine is affected, upper and lower extremities will show signs of dysfunction.[6] If the infection is in the lumbar, deficits are localized to the lower extremities and sacral area.[6] These neurological symptoms are caused by direct pressure on nerves, invasion of neural tissue, tuberculous meningitis, dislocation or subluxation of vertebrae, or reduced blood flow to the spinal cord.[6] Deficits progress from the front to the back, thus affecting the front of the spinal tract first.[6] It heightens reflex and upper motor neuron deficit causing it to eventually advance to limb weakness and difficulty walking due to muscle spasms.[6]
Pott's disease presents in children more frequently due to the increased vascularization of their spine. It also presents with back pain, neurological deficits, cold abscesses, and kyphosis deformities.[6] In children, kyphosis is not limited to the disease being active, instead it increases or worsens in periods of growth, which further exacerbates other symptoms.[6]
Certain presentations can cause abscesses to form, which puts the patient at a higher risk of spinal cord damage and possible paraplegia.[6] The lesions responsible for abscesses occur more frequently in younger patients as their spine is highly vascularized compared to adults.[6] Involvement of the front part of the spine or areas not involving the bone initially spares it and the disc of the spinal column.[6] However, abscess formation allows disease to spread over multiple contiguous vertebrae using the front longitudinal ligament.[6] These abscesses are granulomatous and, as they expand, lift the periosteum leading to bone devascularization, necrosis, and eventually deformity.[6] Rear involvement follows a similar process but uses the longitudinal ligament in the back and often affects the neural arch.[6] Paradiscal, central, and non-bone lesions account for 98% of all spinal TB cases, indicating that lesions originating in the back are much more rare.[6]
Cold abscesses develop near lesions, and they are called 'cold' because they lack typical inflammatory signs like warmth and redness.[5][6] They can grow significantly large which worsens the patient's symptoms.[6] For example, if the primary lesion is located in the cervical spine, a cold abscess could form in the area behind the pharynx causing symptoms such as difficulty swallowing, breathing issues, or a hoarse voice.[6]
Pathogenesis
editInfection of the lungs by the bacteria Mycobacterium tuberculosis (MTB) eventually spreads through the host's body.[6][3] Without treatment and diagnosis, the infection becomes dormant in the lungs or spreads to other parts of the body through hematogenous dissemination.[6]
When dissemination occurs, MTB enters the cancellous or spongy bone of the vertebra through the vascular system.[6] It travels specifically from the front and back spinal arteries, and pressures within the torso spreads the infection throughout the vertebral body.[6][5]
It impacts the front of the vertebral body along the subchondral plate.[3] As it advances, progressive destruction occurs leading to vertebral collapse and kyphosis. The spinal canal may become narrowed due to abscesses, granulation tissue, or direct dural invasion resulting in compression of cord and neurological deficits.[3] Kyphosis is a result of the front of the spine collapsing. Injury to the thoracic spine are more likely to result in kyphosis compared to lumbar spine injuries.[3] A cold abscess can develop if infection spreads to ligaments and soft tissues.[6][3] In the lower back, there is a chance the abscess can move down along the psoas muscle to the upper thigh and eventually break through the skin.[3]
Transmission
editMTB is contracted and spread through aerosol droplets.[6] Respiratory MTB or tuberculosis (TB) have been documented in patients that have negative results for specific cultures.[7] The sum of two cases concluded that about 17% of transmission occurs from patients who have negative results.[7] Another study concluded that TB infection outside the lungs increased the transmission rate, which has always been overlooked.[7]
Risk factors
editSome known risk factors for Pott's Disease include immunodeficiencies (such as those caused by alcohol and drug abuse or HIV), exposure to infected patients, poverty, undernourishment, and lower socioeconomic status.
HIV has been identified as one of the primary risk factors for the development of Pott’s Disease and this is becauseHIV compromises the immune system by attacking and destroying crucial immune cells, thereby weakening the body's natural defenses. This impairment significantly reduces the body's ability to combat infections, including tuberculosis (TB), making it more difficult for the body to fight off TB germs effectively.[8] In regions like Sub-Saharan Africa, where the disease is prevalent, HIV often coexists with spinal TB, significantly complicating management and diagnosis. Data collected in New York and Los Angeles shows that this disease primarily affects foreign-born individuals, African Americans, Asian Americans, and Hispanic Americans.[citation needed]
Vitamin D deficiency has also been correlated with an increased risk of Pott’s Disease, particularly spinal TB with caseous necrosis, increasing the risk of necrosis compared to individuals with normal vitamin D levels. A deficiency in vitamin D has been associated with the activation of tuberculosis (TB) for a long time. TB patients typically have lower serum vitamin D levels compared to healthy individuals. Extended TB treatment also leads to a reduction in serum vitamin D levels. Research has indicated that vitamin D plays a crucial role in modulating innate immune responses, acting as a cofactor in the induction of antimycobacterial activity.[9]
In developed countries like the United States, Pott's Disease is primarily found in adults. However, in developing countries, data shows that Pott's Disease occurs mainly in young adults and older children.[10] Crowded and poorly ventilated living and working conditions, which are often linked to poverty, significantly increase the risk of tuberculosis transmission. Undernutrition is another crucial factor that raises the likelihood of developing active TB. Additionally, poverty correlates with limited health knowledge and a lack of empowerment to utilize that knowledge, which results in greater exposure to various TB risk factors, including HIV, smoking, and alcohol abuse.[11]
Epidemiology
editAbout 2% of all cases of tuberculosis are considered Pott's Disease [12] and about half (50%) of the cases of musculoskeletal tuberculosis are Pott's Disease,[6][13] of which 98% affect the anterior column. The disease can be attributed to 1.3 million deaths per year. There is a correlation between tuberculosis infections and cases of Pott's disease, as it's prevalent in areas where tuberculosis infections are common. Known risk factors like lower socioeconomic status, overcrowding, immunodeficiency, and interactions with people with tuberculosis can influence the rate of diagnosis.[14]
Underdeveloped countries have a higher incidence rate of Pott's disease as it is associated with less ventilated rooms, crowded spaces, poorer hygiene, and less access to healthcare facilities. Increasing food security, reducing poverty, and improving living and working conditions will help to prevent infection and generally enhance the care of those sick.
Pott's disease is more common in the working-age population. Still any age group is at risk for developing the disease.[citation needed] Individuals who have use immunosuppressants or have compromised immune systems, chronic diseases like diabetes, or use tobacco have a significantly increased risk of becoming ill with tuberculosis infections.[15] In older populations, the disease is often misdiagnosed, often being disregarded for other degenerative diseases. Children's spines contain more cartilage, increasing the effect of spinal deformations caused by the disease. [citation needed]
Multidrug resistant tuberculosis poses a threat to people with Pott's disease, making it difficult to determine infection in people because of the paucibacillary symptoms of the disease. Cases of tuberculosis have been on the decline; however, infections of multidrug resistant tuberculosis have remained constant since the 1990s.[citation needed]
Prevention
editAs one type of tuberculosis infections, individuals can’t entirely prevent Pott’s Disease, but we are able to take steps to reduce the risk of TB (tuberculosis) infection by avoiding prolonged, close contact with someone who has an active TB (tuberculosis) infection and getting tested regularly for TB (tuberculosis) if you're at higher risk or live in a region where TB (tuberculosis) is common.[16]
Controlling the spread of tuberculosis infection can prevent tuberculous spondylitis and arthritis. Patients who have a positive PPD test (but not active tuberculosis) may decrease their risk by properly taking medicines to prevent tuberculosis. To effectively treat tuberculosis, patients must take their medications exactly as prescribed.[2]
Management
editWhen it comes to treatment of Pott's disease, the two main routes that are typically prescribed to patients are chemotherapy and surgical intervention.[17] Guidelines from the WHO, CDC, and American Thoracic Society all present chemotherapy to be the first line when it comes to treatment of Pott's disease with surgical interventions being administered as needed for patients who are indicated for it.[17] Antibiotics may also be recommended to help with the eradication of the disease.[17][18] With early intervention, Pott's disease can be cured and completely eradicated from the patient.[16][19] However, there are cases where the tuberculosis is drug-resistant, leading to poorer and possibly life-threatening outcomes in children, the elderly, and immunocompromised patients. Rehabilitation for patients who have just undergone surgery or are recovering from Pott's disease often consist of analgesics for pain management, immobilization of the affected spinal region, and physical therapy for pain-relieving modalities.[20][21]
Chemotherapy
editThe treatment prescribed to patients diagnosed with Pott's disease is similar to treatment that is generally given to patients who have other forms of extrapulmonary tuberculosis.[17] According to guidelines, typical treatment begins with a six to nine month course of chemotherapy.[17][22] The regimen usually consists of an initial 2-month intensive phase of Isoniazid (INH), Rifampin (RIF), Pyrazinamide (PZA), and Ethambutol (EMB).[17] Following the 2-month initial phase, PZA and EMB are discontinued while INH and RIF are continued for the remaining four to seven month continuation phase of the treatment period.[17]
Some practices, however, have recommended treatment regimens of over 12 months given the mortality and disability risks associated with failure to completely eradicate the disease, and the difficulty in assessing the effectiveness of treatment.[22]
Surgical intervention
editSurgical intervention is required for patients with Pott's disease in the event that there is a need for tissue sampling to clarify diagnoses, resistance to chemotherapy (often found in patients with HIV), neurologic deficits (including but not limited to abnormal reflexes, problems with speech, decreased sensation, loss of balance, decreased mental function, vision/hearing problems, and paraplegia), paravertebral abscesses formed from bacterial induced immune response, and kyphotic deformities leading to instability of the spine.[23] However, surgery is up to shared clinical decision making and not an intervention that is defaulted to, as guidelines tend to lead towards less invasive procedures such as chemotherapy and anti-tuberculosis medications.[24]
Typical surgical techniques used are as follows:
- Posterior decompression and fusion with bone autografts[23][25]
- Anterior debridement/decompression and fusion with bone autografts[23][25]
- Anterior debridement/decompression and fusion followed by simultaneous or sequential posterior fusion with instrumentation[23][25]
- Posterior fusion with instrumentation followed by simultaneous or sequential anterior debridement/decompression and fusion[23][25]
Posterior decompression and fusion
editIn posterior decompression and fusion with bone autografts, the goal is to relieve pressure on the spinal cord and nerves in the lower back and prevent the progression of kyphosis in active disease.[26][27] In this procedure, the lumbar (lower back) vertebrae (L1-L5) are exposed and the intervertebral discs and vertebral material impinging on the spinal cord and/or nerves are removed.[26] The vertebrae (typically L4-L5 due to their load bearing nature and vulnerability to degradation) are then fused together with grafts or instrumentation to help provide more support to the back and spine of the patient.[26]
Anterior debridement/Decompression and fusion
editThe goal of the anterior debridement/decompression and fusion with bone autografts procedure is to relieve pressure on the spinal cord and nerves along the anterior side of the spinal cord and help prevent the progression of kyphosis in active disease.[27][28] The anterior approach is often recommended instead of the posterior approach in cases where only single segments of the vertebrae are affected, and in the event that there is no destruction or collapse of the posterior elements.[28] In anterior debridement and decompression, tissue damaged by the onset of disease is removed along with vertebral elements and intervertebral discs that are impinging on the spinal cord and/or nerves in the spine.[28] Vertebrae can then be fused together through the use of grafts or instrumentation to provide more structural support for the spine and back.[28]
Kyphosis progression prevention
editSurgical intervention is used in patients with kyphosis to primarily prevent the progression of kyphosis in active disease and correct it to a certain extent.[27] However, surgical intervention is not meant to cure kyphosis in the patient and has variable rates of success in eradicating it in a patient.[27] In the event that a patient shows signs of kyphosis, the earlier surgical intervention is given, the better the outcome for the patient.[27]
Pediatric surgical interventions
editIn children with Pott's disease, earlier surgical intervention is often recommended to reduce their increased risk for kyphotic deformity.[23] This increased risk for deformity is attributed to both the anatomy and biomechanics of children and their developmental stage of life.[23][29] Due to the proportions of their bodies (larger head), limited muscular development, and increased flexibility, gravity can lead to greater deformation and presentation of kyphosis.[29] After onset of the disease, growth plates in the spine may be destroyed and vertebral bodies suppressed due to kyphosis.[29] These variable complications would then further deformation, leading to uncontrolled and/or suppressed growth.[29]
Prognosis
edit- Paraplegia (so-called Pott's paraplegia), presents with refusal to stand or walk. It can generally be used to describe those who have lost feeling in their lower extremities/lower parts of the body or are unable to move them.[30]
- Vertebral collapse resulting in kyphosis, which is defined as an abnormally curved thoracic spine. This abnormal curve in the spine is not to be confused with the natural curve which serves to absorb shock. The main presentation of kyphosis is gradual onset of pain in patients that may be worse with activity.[31]
- Sinus formation is a complex form of recurrent tuberculosis.[32]
- Spinal cord compression occurs and can stop the nerves from functioning properly when pressure builds on the spinal cord. The consequence of this compression and pressure is symptoms such as back pain, trouble walking, and weakness in the arms and/or legs.[33][34]
History
editEvidence of tubercular lesions of the vertebral column have been found from the fourth millennium BC in the form of Mesolithic remains in Liguria, Italy. Additionally, tuberculosis spondylitis has been discovered from 3400 BC in the mummified remains of Egyptians. Tuberculosis had affected humans long before it was identified by Sir Percivall Pott.[35]
Important milestones in the development, understanding, and management of tuberculosis spondylitis include the Bacilli Calmette Guerin (BCG) vaccination in 1945, radiological exams, and accessibility of necessary anti tubular medications in the mid 1900's.[1] MRI and CT scans implemented since 1987 for this disease have helped clinicians catch the disease early as well as identify rare complications of the disease. This helps to prevent further worsening of the disease and promote proper management.[36]
- Saint Gemma of Lucca had tuberculosis of the spine.
- English poets Alexander Pope and William Ernest Henley both had Pott disease.
- Anna Roosevelt Cowles, sister of President Theodore Roosevelt, had Pott disease.
- Søren Kierkegaard may have died from Pott disease, according to professor Kaare Weismann and literature scientist Jens Staubrand[37]
- Chick Webb, a swing-era drummer and band leader, was affected by tuberculosis of the spine as a child, which left him hunchbacked, and eventually caused his death.
- The Sicilian mafia boss Luciano Leggio had the disease and wore a brace.
- Italian writer, poet, and philosopher Giacomo Leopardi had the disease.
- American actor Pat Morita was hospitalized as a child with the disease, and when he recovered, was sent directly to an internment camp.
- It features prominently in the book This Is a Soul, which chronicles the work of American physician Rick Hodes in Ethiopia.
- Jane Addams, social activist and Nobel Peace Prize winner, had Pott disease.
- Willem Ten Boom, brother of Corrie Ten Boom, died of tuberculosis of the spine in December 1946.[38]
- Writer Max Blecher had Pott disease and wrote about the affliction.
- Marxist thinker and Communist leader Antonio Gramsci had Pott disease which, together with the bad conditions of his incarceration in fascist Italy during the 1930s, contributed to his death.
- Gavrilo Princip, who assassinated Archduke Franz Ferdinand of Austria, leading to World War I, died in prison of bone tuberculosis.
- English writer Denton Welch (1915–1948) died of spinal tuberculosis after being involved in a motor accident (1935) that irreparably damaged his spine.
- Louis Joseph, Dauphin of France, son of King Louis XVI and Marie Antoinette[39]
- George Mercer Dawson, Canadian surveyor, geologist and president of the Geological Society of America, had Pott's disease.
- Masaoka Shiki, Japanese poet, author and literary critic, had Pott's disease.
In popular culture
edit- Max Blecher's semi-autobiographical novel Inimi cicatrizate (1937) is about a young man named Emanuel who is afflicted with Pott disease in a sanatorium, as is the Radu Jude film Scarred Hearts (2016), loosely based on it.
- A. J. Cronin's story "Two Gentlemen of Verona," includes a character named Lucia with tuberculosis of spine.
- In William Golding's novel The Spire (1964), Jocelin, the dean who wanted a spire on his cathedral, probably dies as a result of the disease.
- Katharine Butler Hathaway's memoir The Little Locksmith (1943) is about the effects of spinal tuberculosis on her childhood and adult life.
- In Victor Hugo's The Hunchback of Notre-Dame (1831) the title character has a gibbus deformity similar to the type caused by spinal tuberculosis.
- In Henrik Ibsen's play A Doll's House (1879), Dr. Rank has "consumption of the spine."
- In Sergio Leone's film Once Upon a Time in the West (1968), Morton, the railroad magnate, has the disease and needs crutches to walk.
- In Ernest Poole's Pulitzer Prize-winning novel, His Family (1917), young Johnny Geer has a terminal case of Pott disease.
- In Edmund Wilson's Memoirs of Hecate County (1946), the novella "The Princess with the Golden Hair," has a character with Pott disease.
References
edit- ^ a b Tuli SM (June 2013). "Historical aspects of Pott's disease (spinal tuberculosis) management". European Spine Journal. 22 (Suppl 4): 529–538. doi:10.1007/s00586-012-2388-7. PMC 3691412. PMID 22802129.
- ^ a b Garg RK, Somvanshi DS (2011). "Spinal tuberculosis: a review". The Journal of Spinal Cord Medicine. 34 (5): 440–454. doi:10.1179/2045772311Y.0000000023. PMC 3184481. PMID 22118251.
- ^ a b c d e f g Pott Disease (Tuberculous Spondylitis) at eMedicine
- ^ Wong-Taylor LA, Scott AJ, Burgess H (May 2013). "Massive TB psoas abscess". BMJ Case Reports. 2013: bcr2013009966. doi:10.1136/bcr-2013-009966. PMC 3670072. PMID 23696148.
- ^ a b c d e f g h i j k Ansari S, Amanullah MF, Rauniyar R, Ahmad K (2013). "Pott′s spine: Diagnostic imaging modalities and technology advancements". North American Journal of Medical Sciences. 5 (7): 404–411. doi:10.4103/1947-2714.115775. PMC 3759066. PMID 24020048.
- ^ a b c d e f g h i j k l m n o p q r s t u v w x y z Glassman I, Nguyen KH, Giess J, Alcantara C, Booth M, Venketaraman V (January 2023). "Pathogenesis, Diagnostic Challenges, and Risk Factors of Pott's Disease". Clinics and Practice. 13 (1): 155–165. doi:10.3390/clinpract13010014. PMC 9955044. PMID 36826156.
- ^ a b c Schirmer P, Renault CA, Holodniy M (August 2010). "Is spinal tuberculosis contagious?". International Journal of Infectious Diseases. 14 (8): e659–666. doi:10.1016/j.ijid.2009.11.009. PMID 20181507.
- ^ CDC (2024-06-17). "TB Risk and People with HIV". Tuberculosis (TB). Retrieved 2024-08-01.
- ^ Talat N, Perry S, Parsonnet J, Dawood G, Hussain R (May 2010). "Vitamin D Deficiency and Tuberculosis Progression". Emerging Infectious Diseases. 16 (5): 853–855. doi:10.3201/eid1605.091693. PMC 2954005. PMID 20409383.
- ^ Piña-Garza JE (2013-01-01), Piña-Garza JE (ed.), "Chapter 12 - Paraplegia and Quadriplegia", Fenichel's Clinical Pediatric Neurology (Seventh Edition), London: W.B. Saunders, pp. 253–269, doi:10.1016/b978-1-4557-2376-8.00012-8, ISBN 978-1-4557-2376-8, retrieved 2024-08-01
- ^ Hickey KT, Masterson Creber RM, Reading M, Sciacca RR, Riga TC, Frulla AP, et al. (August 2018). "Low health literacy: Implications for managing cardiac patients in practice". The Nurse Practitioner. 43 (8): 49–55. doi:10.1097/01.NPR.0000541468.54290.49. ISSN 0361-1817. PMC 6391993. PMID 30028773.
- ^ Ansari S, Amanullah MF, Rauniyar R, Ahmad K (2013). "Pott′s spine: Diagnostic imaging modalities and technology advancements". North American Journal of Medical Sciences. 5 (7): 404–411. doi:10.4103/1947-2714.115775. ISSN 1947-2714. PMC 3759066. PMID 24020048.
- ^ Manno RL, Yazdany J, Tarrant TK, Kwan M (2022). Current Medical Diagnosis & Treatment 2023. McGraw Hill Education. ISBN 978-1-2646-8734-3.[page needed]
- ^ Viswanathan VK, Subramanian S (2024). "Pott Disease". StatPearls. Treasure Island (FL): StatPearls Publishing. PMID 30855915. Retrieved 2024-07-25.
- ^ "Tuberculosis (TB)". www.who.int. Retrieved 2024-07-31.
- ^ a b Pan Z, Cheng Z, Wang JC, Zhang W, Dai M, Zhang B (September 2021). "Spinal Tuberculosis: Always Understand, Often Prevent, Sometime Cure". Neurospine. 18 (3): 648–650. doi:10.14245/ns.2142788.394. PMC 8497242. PMID 34610698.
- ^ a b c d e f g Nahid P, Dorman SE, Alipanah N, Barry PM, Brozek JL, Cattamanchi A, et al. (October 2016). "Official American Thoracic Society/Centers for Disease Control and Prevention/Infectious Diseases Society of America Clinical Practice Guidelines: Treatment of Drug-Susceptible Tuberculosis". Clinical Infectious Diseases. 63 (7): e147–e195. doi:10.1093/cid/ciw376. PMC 6590850. PMID 27516382.
- ^ Rajasekaran S, Soundararajan D, Shetty AP, Kanna RM (December 2018). "Spinal Tuberculosis: Current Concepts". Global Spine Journal. 8 (4_suppl): 96S–108S. doi:10.1177/2192568218769053. PMC 6295815. PMID 30574444.
- ^ Patankar A (September 2016). "Tuberculosis of spine: An experience of 30 cases over two years". Asian Journal of Neurosurgery. 11 (3): 226–231. doi:10.4103/1793-5482.145085. PMC 4849291. PMID 27366249.
- ^ Dhouibi J, Kalai A, Chaabeni A, Aissa A, Ben Salah Frih Z, Jellad A (2024-04-04). "Rehabilitation management of patients with spinal tuberculosis (Review)". Medicine International. 4 (3): 28. doi:10.3892/mi.2024.152. PMC 11040281. PMID 38660125.
- ^ Jain AK, Jain S (February 2012). "Instrumented stabilization in spinal tuberculosis". International Orthopaedics. 36 (2): 285–292. doi:10.1007/s00264-011-1296-5. PMC 3282857. PMID 21720864.
- ^ a b Lee JY (April 2015). "Diagnosis and treatment of extrapulmonary tuberculosis". Tuberculosis and Respiratory Diseases. 78 (2): 47–55. doi:10.4046/trd.2015.78.2.47. PMC 4388900. PMID 25861336.
- ^ a b c d e f g Rasouli MR, Mirkoohi M, Vaccaro AR, Yarandi KK, Rahimi-Movaghar V (December 2012). "Spinal tuberculosis: diagnosis and management". Asian Spine Journal. 6 (4): 294–308. doi:10.4184/asj.2012.6.4.294. PMC 3530707. PMID 23275816.
- ^ Jutte PC, Van Loenhout-Rooyackers JH (January 2006). "Routine surgery in addition to chemotherapy for treating spinal tuberculosis". The Cochrane Database of Systematic Reviews. 2006 (1): CD004532. doi:10.1002/14651858.CD004532.pub2. PMC 6532687. PMID 16437489.
- ^ a b c d Okada Y, Miyamoto H, Uno K, Sumi M (November 2009). "Clinical and radiological outcome of surgery for pyogenic and tuberculous spondylitis: comparisons of surgical techniques and disease types: Clinical article". Journal of Neurosurgery: Spine. 11 (5): 620–627. doi:10.3171/2009.5.SPINE08331. PMID 19929368.
- ^ a b c Jun DS, Yu CH, Ahn BG (September 2011). "Posterior direct decompression and fusion of the lower thoracic and lumbar fractures with neurological deficit". Asian Spine Journal. 5 (3): 146–154. doi:10.4184/asj.2011.5.3.146. PMC 3159062. PMID 21892386.
- ^ a b c d e Jain AK, Dhammi IK, Jain S, Mishra P (April 2010). "Kyphosis in spinal tuberculosis - Prevention and correction". Indian Journal of Orthopaedics. 44 (2): 127–136. doi:10.4103/0019-5413.61893. PMC 2856387. PMID 20418999.
- ^ a b c d Anshori F, Priyamurti H, Rahyussalim AJ (2020). "Anterior debridement and fusion using expandable mesh cage only for the treatment of paraparese due to spondylitis tuberculosis: A case report". International Journal of Surgery Case Reports. 77: 191–197. doi:10.1016/j.ijscr.2020.10.126. PMC 7652712. PMID 33166818.
- ^ a b c d Govender S, Ramnarain A, Danaviah S (July 2007). "Cervical spine tuberculosis in children". Clinical Orthopaedics and Related Research. 460: 78–85. doi:10.1097/BLO.0b013e31806a915f. PMID 17620809.
- ^ "About Spinal Cord Injury". Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD). U.S. National Library of Medicine. 2022-01-25. Retrieved 2024-07-26.
- ^ "Kyphosis". pp. 119–120. in: Ebert JR (2008). "Back, Hip, and Knee Disorders". Adolescent Medicine. pp. 117–131. doi:10.1016/B978-032304073-0.10018-4. ISBN 978-0-323-04073-0.
- ^ Wang B, Kong L, Zhu Z, Gao W, Guo H, Wang X, et al. (2018-05-02). "Recurrent complex spinal tuberculosis accompanied by sinus tract formation: causes of recurrence and clinical treatments". Scientific Reports. 8 (1): 6933. Bibcode:2018NatSR...8.6933W. doi:10.1038/s41598-018-25142-z. ISSN 2045-2322. PMC 5932000. PMID 29720686.
- ^ Alruwaili A, Umerani M, Darwish A, Mostafa G (2020). "Neurological recovery after early decompression for dorsal Pott's spine". International Journal of Surgery Case Reports. 66: 236–239. doi:10.1016/j.ijscr.2019.12.008. PMC 6931094. PMID 31874383.
- ^ Zeidman SM, Ducker TB (2005), "Infectious Complications of Spine Surgery", Spine Surgery, Elsevier, pp. 2013–2026, doi:10.1016/b978-0-443-06616-0.50159-0, ISBN 978-0-443-06616-0
- ^ Khoo LT, Mikawa K, Fessler RG (March 2003). "A surgical revisitation of Pott distemper of the spine". The Spine Journal. 3 (2): 130–145. doi:10.1016/S1529-9430(02)00410-2. PMID 14589227.
- ^ Tuli SM (June 2013). "Historical aspects of Pott's disease (spinal tuberculosis) management". European Spine Journal. 22 (S4): 529–538. doi:10.1007/s00586-012-2388-7. ISSN 0940-6719. PMC 3691412. PMID 22802129.
- ^ Krasnik B (2013). "Kierkegaard døde formentlig af Potts sygdom" [Kierkegaard probably died of Pott's disease] (in Danish). Kristeligt Dagblad. Archived from the original on 2016-10-13. Retrieved 2016-10-02.
- ^ Ten Boom C, Sherrill C, Sherrill J (2015). "Since Then". The Hiding Place. Hendrickson Publishers. ISBN 978-1-61970-597-5.
- ^ Covington R. "Marie Antoinette". Smithsonian. Retrieved 2019-08-18.
Further reading
edit- Jodra S, Alvarez C (21 February 2013). "Pott's Disease of the Thoracic Spine". New England Journal of Medicine. 368 (8): 756. doi:10.1056/NEJMicm1207442. PMID 23425168.
- Bydon A, Dasenbrock HH, Pendleton C, McGirt MJ, Gokaslan ZL, Quinones-Hinojosa A (August 2011). "Harvey Cushing, the Spine Surgeon: The Surgical Treatment of Pott Disease". Spine. 36 (17): 1420–1425. doi:10.1097/BRS.0b013e3181f2a2c6. PMC 4612634. PMID 21224751.
- Radcliffe C, Grant M (9 September 2021). "Pott Disease: A Tale of Two Cases". Pathogens. 10 (9): 1158. doi:10.3390/pathogens10091158. PMC 8465804. PMID 34578190.
- Alajaji NM, Sallout B, Baradwan S (9 May 2022). "A 27-Year-Old Woman Diagnosed with Tuberculous Spondylitis, or Pott Disease, During Pregnancy: A Case Report". American Journal of Case Reports. 23: e936583. doi:10.12659/AJCR.936583. PMC 9195639. PMID 35684941.
External links
editMedia related to Pott's disease at Wikimedia Commons