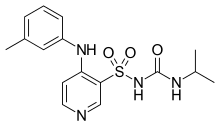
Torasemide, also known as torsemide, is a diuretic medication used to treat fluid overload due to heart failure, kidney disease, and liver disease. It is a less preferred treatment for high blood pressure.[1] It is taken by mouth or by injection into a vein.[1]
 | |
| Clinical data | |
|---|---|
| Trade names | Demadex, Tortas, Wator |
| Other names | Torsemide, Torsemide (USAN US) |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a601212 |
| License data | |
| Routes of administration | By mouth, intraveneous |
| Drug class | Loop diuretic |
| ATC code | |
| Legal status | |
| Legal status |
|
| Pharmacokinetic data | |
| Bioavailability | 80-90% |
| Protein binding | Highly bound (>99%). |
| Metabolism | Liver (80%) |
| Elimination half-life | 3.5 hours; Cirrhosis: 7-8 hours |
| Identifiers | |
| |
| CAS Number | |
| PubChem CID | |
| IUPHAR/BPS | |
| DrugBank | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| CompTox Dashboard (EPA) | |
| ECHA InfoCard | 100.164.924 |
| Chemical and physical data | |
| Formula | C16H20N4O3S |
| Molar mass | 348.42 g·mol−1 |
| 3D model (JSmol) | |
| |
| |
| | |
Common side effects include headache, increased urination, diarrhea, cough, and dizziness.[1] Other side effects may include hearing loss and low blood potassium.[1] Torasemide is a sulfonamide and loop diuretic.[1] Use is not recommended in pregnancy or breastfeeding.[2] It works by decreasing the reabsorption of sodium by the kidneys.[1]
Torasemide was patented in 1974 and came into medical use in 1993.[3] It is on the World Health Organization's List of Essential Medicines.[4] It is available as a generic medication.[2] In 2022, it was the 184th most commonly prescribed medication in the United States, with more than 2 million prescriptions.[5][6]
Medical uses
editIt is used to treat fluid overload due to heart failure. It is sometimes used to treat high blood pressure.[1] Compared with furosemide, torasemide is associated with a lower risk of rehospitalization for heart failure and an improvement in New York Heart Association class of heart failure.[7][8][9] In heart failure it may be safer and more effective than furosemide.[10][11][12] Long-term outcomes with torasemide may be better than with furosemide in patients with heart failure.[13]
Adverse effects
editNo evidence of torasemide-induced ototoxicity has been demonstrated in humans.[14]
Loop diuretics, including torsemide, may decrease total body thiamine, particularly in people with poor thiamine intake, and this depletion may worsen heart failure. It is therefore reasonable to either also give thiamine supplements or to check blood thiamine levels in those being treated with chronic loop diuretics.[15]
Chemistry
editCompared with other loop diuretics, torasemide has a more prolonged diuretic effect than equipotent doses of furosemide and relatively decreased potassium loss.[16]
Names
editTorasemide is the recommended name of the drug (rINN) according to the (INN), which is the drug naming system coordinated by the World Health Organization. Torsemide is the official name of the drug according to the (USAN), which is the drug naming system coordinated by the USAN Council, which is co-sponsored by the American Medical Association (AMA), the United States Pharmacopeial Convention (USP), and the American Pharmacists Association (APhA).
Veterinary uses
editIn May 2024, the US FDA conditionally approved the first torsemide animal medication for dogs. UpCard-CA1 (torsemide oral solution) was conditionally approved for use with concurrent therapy with pimobendan, spironolactone, and an angiotensin-converting enzyme (ACE) inhibitor for the management of pulmonary edema (fluid build-up in lungs) in dogs with congestive heart failure caused by myxomatous mitral valve disease (MMVD).[17][18]
References
edit- ^ a b c d e f g "Torsemide Monograph for Professionals". Drugs.com. American Society of Health-System Pharmacists. Retrieved 18 March 2019.
- ^ a b British national formulary : BNF 76 (76 ed.). Pharmaceutical Press. 2018. pp. 227–228. ISBN 978-0-85711-338-2.
- ^ Fischer J, Ganellin CR (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 458. ISBN 978-3-527-60749-5.
- ^ World Health Organization (2021). World Health Organization model list of essential medicines: 22nd list (2021). Geneva: World Health Organization. hdl:10665/345533. WHO/MHP/HPS/EML/2021.02.
- ^ "The Top 300 of 2022". ClinCalc. Archived from the original on 30 August 2024. Retrieved 30 August 2024.
- ^ "Torsemide Drug Usage Statistics, United States, 2013 - 2022". ClinCalc. Retrieved 30 August 2024.
- ^ Abraham B, Megaly M, Sous M, Fransawyalkomos M, Saad M, Fraser R, et al. (January 2020). "Meta-Analysis Comparing Torsemide Versus Furosemide in Patients With Heart Failure". Am. J. Cardiol. 125 (1): 92–99. doi:10.1016/j.amjcard.2019.09.039. PMID 31699358. S2CID 207937875.
- ^ Täger T, Fröhlich H, Seiz M, Katus HA, Frankenstein L (March 2019). "READY: relative efficacy of loop diuretics in patients with chronic systolic heart failure-a systematic review and network meta-analysis of randomised trials". Heart Fail Rev. 24 (4): 461–472. doi:10.1007/s10741-019-09771-8. PMID 30874955. S2CID 77394851.
- ^ Miles JA, Hanumanthu BK, Patel K, Chen M, Siegel RM, Kokkinidis DG (June 2019). "Torsemide versus furosemide and intermediate-term outcomes in patients with heart failure: an updated meta-analysis". J Cardiovasc Med (Hagerstown). 20 (6): 379–388. doi:10.2459/JCM.0000000000000794. PMID 30950982. S2CID 96436158.
- ^ Wargo KA, Banta WM (November 2009). "A comprehensive review of the loop diuretics: should furosemide be first line?". Ann Pharmacother. 43 (11): 1836–47. doi:10.1345/aph.1M177. PMID 19843838. S2CID 43339236.
- ^ Roush GC, Kaur R, Ernst ME (2014). "Diuretics: a review and update". J. Cardiovasc. Pharmacol. Ther. 19 (1): 5–13. doi:10.1177/1074248413497257. PMID 24243991. S2CID 21204143.
- ^ Buggey J, Mentz RJ, Pitt B, Eisenstein EL, Anstrom KJ, Velazquez EJ, et al. (2015). "A reappraisal of loop diuretic choice in heart failure patients". Am. Heart J. 169 (3): 323–33. doi:10.1016/j.ahj.2014.12.009. PMC 4346710. PMID 25728721.
- ^ Ozierański K, Balsam P, Kapłon-Cieślicka A, Tymińska A, Kowalik R, Grabowski M, et al. (February 2019). "Comparative Analysis of Long-Term Outcomes of Torasemide and Furosemide in Heart Failure Patients in Heart Failure Registries of the European Society of Cardiology". Cardiovascular Drugs and Therapy. 33 (1): 77–86. doi:10.1007/s10557-018-6843-5. hdl:2183/22704. PMID 30649675. S2CID 58014640.
- ^ Dunn CJ, Fitton A, Brogden RN (January 1995). "Torasemide. An update of its pharmacological properties and therapeutic efficacy". Drugs. 49 (1): 121–42. doi:10.2165/00003495-199549010-00009. PMID 7705212. S2CID 261404564.
- ^ Kattoor AJ, Goel A, Mehta JL (August 2018). "Thiamine Therapy for Heart Failure: a Promise or Fiction?". Cardiovasc Drugs Ther. 32 (4): 313–317. doi:10.1007/s10557-018-6808-8. PMID 30022355.
- ^ Christopher J. Dunn (1995). "Torasemide: An Update of its Pharmacological Properties and Therapeutic Efficacy". Drugs. 49 (1): 121–142. doi:10.2165/00003495-199549010-00009. PMID 7705212. Retrieved 8 March 2024.
- ^ "FDA Conditionally Approves First Torsemide Animal Drug for Dogs". U.S. Food and Drug Administration (Press release). 10 May 2024. Retrieved 15 May 2024. This article incorporates text from this source, which is in the public domain.
- ^ "FDA Roundup: May 14, 2024". U.S. Food and Drug Administration (Press release). 14 May 2024. Retrieved 15 May 2024. This article incorporates text from this source, which is in the public domain.